The bacteria Neisseria meningitidis, also called meningococcus, causes meningococcal meningitis worldwide. However, Haemophilus influenzae type b (Hib) and Streptococcus pneumoniae are the main contributors to bacterial meningitis in Malaysia where the vaccine for Hib is already included in the National Immunisation Programme (NIP). Unfortunately, the meningococcal vaccine is not routinely recommended and neither is the pneumococcal vaccine.
What Is Meningitis?
The bacteria Neisseria meningitidis only infect humans and 10% to 20% of the population are asymptomatic carriers of this bacteria. N.meningitidis is transmitted from person-to-person through droplets of respiratory (i.e. kissing, sneezing or coughing) or throat secretions from carriers.
The illness occurs when the bacteria break through the protective lining of the nose and throat and enter the bloodstream. Once in the bloodstream, they multiply rapidly, overwhelming the body’s defences thus allowing bacteria to cross the blood-brain barrier infecting the meninges, causing meningitis.
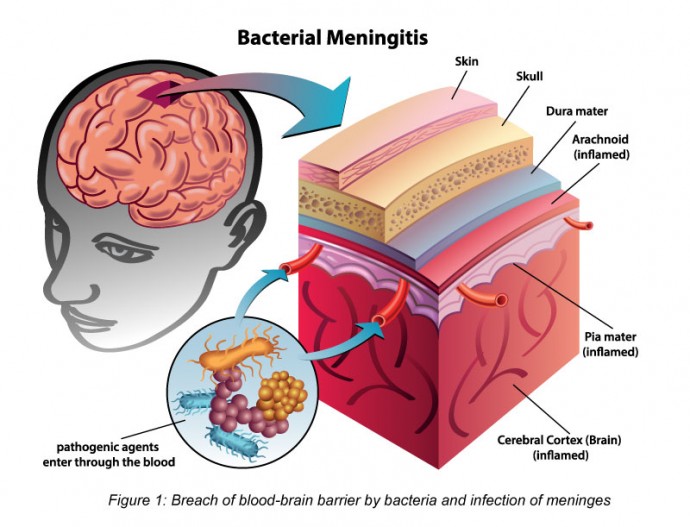
THE MENINGES
Meninges refers to three membranes (the dura mater, arachnoid, and pia mater) that line the skull and enclose the brain and spinal cord. Its primary function is to protect the central nervous system.
High Risk Groups & Risk Factors
Infants less than one year and people ages 16 through 23 years are more likely to be infected than other age groups, but cases occur in all age groups including the elderly. Additionally, travellers, especially those headed to the so-called ‘meningitis belt’ in Africa and pilgrims of the Hajj are similarly at risk.
Meanwhile, some risk factors for the disease can include:
- Household or dormitory crowding
- Active and passive smoking
- Previous case of upper respiratory tract infection
- Chronic underlying illness (e.g. liver failure, lupus)
- Dysfunctional or absence of a spleen
- Properdin deficiency (a rare, genetically-linked condition where a deficiency of a blood plasma component affects immunity)
- Human immunodeficiency virus (HIV)
Signs & Symptoms of Infection in Children
The average incubation period of the bacteria is 4 days – which is fast, but the disease progression is even faster. Therefore, if your child shows any of the symptoms stated below, you should immediately bring him/her to the hospital. Early antibiotic treatment using penicillin, ampicillin, chloramphenicol or ceftriaxone can save lives.
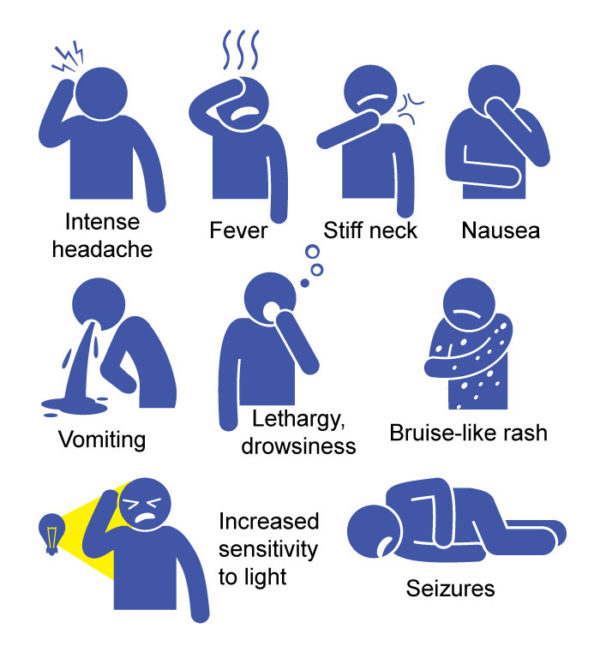
Symptoms often seen in young children:
In newborns and babies, the symptoms of fever, headache, and neck stiffness may be absent or unnoticeable. Instead, they may show signs of irritability, vomiting, poor appetite, or appear to be slow or inactive.
Infection by meningocucus can cause embolisation of bacterial clots causing gangrene of toes, fingers and even limbs that then drop off (auto amputation).
Protecting Your Child
Unfortunately, despite adequate and early treatment, 10-15% of patients die, typically within 24-48 hours after getting infected. Most survivors make a full recovery without long-term effects, however 10-19% of them may suffer from permanent disability (e.g. hearing loss, loss of limb, or neurological damage). Hence, preventing infection through immunisation is preferred.
Malaysia has long approved the use of the meningococcal polysaccharide vaccine which can be used for children starting from 2 years and above. Since the 2002 Hajj meningococcal outbreaks, Saudi health officials require pilgrims to be vaccinated against all 4 main meningococcal serogroups (A, C, Y and W135).
The more recent meningococcal conjugate vaccine (MCV) is far more efficacious and can protect against all 4 main meningococcal serogroups. Unlike its polysaccharide counterpart, MCV can be administered as early as 6 weeks of age and it also prevents carriage of the bacteria. You can get your child vaccinated at clinics or hospitals that provide them but be sure to consult your paediatrician first.
An educational contribution by Malaysian Paediatric Association.





Comments