Pneumonia is one of the top five causes of childhood death in Malaysia according to the Department of Statistics. What makes pneumonia deadly to children?
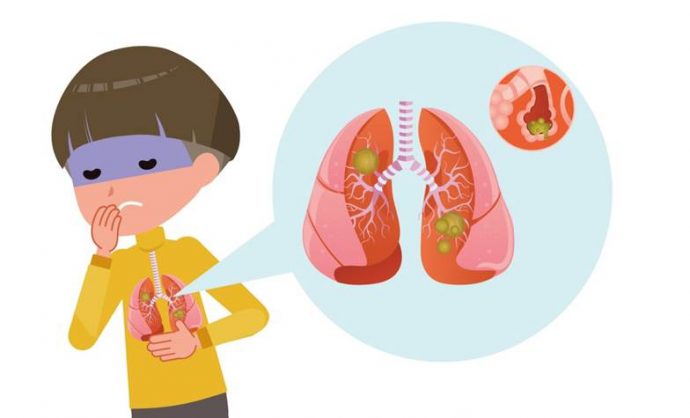
Pneumonia is a lung infection that causes the air sacs (alveoli) in the lungs to fill up with fluid or pus, making it difficult to breathe in enough oxygen for the body. Anyone can get infected, but infants, the aged and sick people are the most vulnerable due to their weaker immune systems.
The burden
Globally, around 1.4 million children under 5 years old die every year because of pneumonia. UNICEF has also reported that only few caregivers recognise pneumonia symptoms and only half of the infected children are given the appropriate treatment. As the symptoms are similar to a common cold or flu, many parents may not realise the severity of their child’s condition until it is too late.
Types of pneumonia
Doctors may categorise pneumonia into how or where the infection started:
- Hospital-acquired pneumonia occurs during a stay in a hospital or when receiving outpatient treatment. The illness can be more severe as the infectious bacteria may be resistant to antibiotics.
- Community-acquired pneumonia starts somewhere other than a hospital or healthcare facility and is more common. This type of pneumonia can be caused by bacteria, viruses, fungi or chemicals.
Cause of illness
Pneumonia is also categorised based on the cause.
- Bacteria. Streptococcus pneumoniae (pneumococcus) is the most common cause of bacterial pneumonia, and also the cause of the highest number of pneumonia-linked deaths in children. Other bacteria include Haemophilus influenzae type B (Hib), Klebsilla pneumoniae, Chlamydia pneumoniae and others.
- Virus. Respiratory syncytial virus (RSV) is the most common cause of viral pneumonia in children. Other viruses include influenza virus (type A and B), rhinovirus (common cold virus), and coronavirus (like COVID-19 and SARS).
- Fungi. Pneumocystis jirovecii is an example of fungi that can cause fungal pneumonia, which is less common and tends to happen to people with chronic health problems or weakened immune systems.
- Chemicals. Different substances in different forms (liquid, gas, small particles) can cause inflammation of the lungs when inhaled. This includes toxic and poisonous chemicals, as well as food and drinks (aspiration pneumonia).
Is it? Is it not?
It can be hard to recognise symptoms in children. Ranging from mild to severe, it also depends on the cause and health status of your child. Symptoms may include:
- Fever
- Cough
- Wheezing
- Rapid breathing
- Trouble breathing
- Skin, lips, or fingertips that look blue
- Symptoms in babies might be vague, like fussiness or trouble feeding
Early treatment is vital
If treatment is delayed, complications may arise.
- Bacteraemia. The infection spreads into the bloodstream, leading to septic shock and blood pressure dropping to a dangerous level.
- Lung abscesses. Pockets of pus may build up in the lungs. The child may also cough out pus and have a high fever.
- Pleurisy. The pleura (two layers of tissue enveloping the lungs) become swollen and cause a sharp chest pain when breathing deeply. If the swelling is untreated, fluid may fill the area between the pleura, causing pleural effusion (“water around the lungs”) and empyema (pus collection).
- Respiratory and organ failure. The lungs may be unable to function properly enough to transfer oxygen to the blood and remove carbon dioxide from the blood. This can be life-threatening as organs such as the kidneys and heart may also fail to function as normal.
Protection against pneumonia
- Protect. Practise proper hygiene and hand-washing, provide optimal nutrition, avoid indoor pollution and smoking, and reduce other risk factors.
- Prevent. Immunisation against pneumococcus, influenza, Hib, measles and pertussis is vital. Vaccines for Hib, measles and pertussis are part of our National Immunisation Programme (NIP) and pneumococcal vaccine will be introduced soon in NIP. The annual influenza vaccine is available in public and private healthcare facilities.
- Treat. Prompt and correct symptom identification is crucial to ensure early and appropriate care, which plays a role in treating pneumonia and preventing further complications and death. If uncertain, it is best to seek doctors’ advice early on to be sure, rather than waiting for your child’s condition to worsen.
For pneumonia, early treatment is crucial for a higher survival rate. In any case, it is best to take protective and preventive measures always.
An educational contribution by Malaysian Paediatric Association.






Comments