Antibiotic-associated diarrhoea (AAD) is the passing of loose, watery stools three or more times a day after taking antibiotics. Mild cases of AAD will spontaneously clear up on its own once the antibiotic course is completed. The leading cause of AAD is an infection by the bacterium Clostridium difficile (C. difficile), that is a toxin-producing bacteria which accounts for around 1 in 5 cases, and can be serious enough to lead to hospitalisation.
How AAD occurs
Antibiotics (which are antibacterial) are medications that affect the bacterial cell structure and hence, have the ability to kill bacteria. However, antibiotics are not able to differentiate between the ‘bad’ and ‘good’ bacteria. AAD occurs because of dysbiosis, i.e. a disruption of the balance of ‘bad’ versus ‘good’ bacteria in the gut that leads to overgrowth of ‘bad’ bacteria.
Nearly all antibiotics can potentially cause AAD, including most of the commonly used broad spectrum types such as cephalosporin and also penicillin.
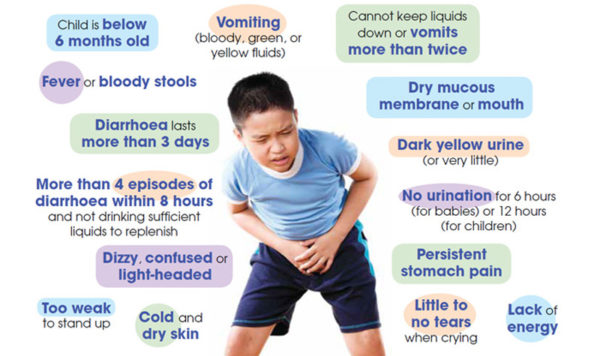
Severe dehydration as a result of AAD is the most serious complication in children. Therefore, always keep your child well-hydrated as severe dehydration can lead to seizures, brain damage, or even death. Mild cases of AAD will not cause significant loss of fluids, but visit the doctor immediately if any of the following symptoms/signs apply:
Preventing AAD
There is some evidence to show that certain probiotics (good bacteria that when consumed in sufficient amounts leads to beneficial results) can help minimise AAD. Each probiotic strain is unique, just like each individual can be uniquely identified by their fingerprints. Thus, certain strains are more effective for treating certain conditions.
When it comes to AAD, bacterial probiotics such as Lactobacillus reuteri, Lactobacillus rhamnosus, and yeast-based probiotics such as Saccharomyces boulardii have been shown to be useful. Unlike the bacterial probiotics, Saccharomyces boulardii is highly recommended in the event of AAD with C. difficile infection as it has a proven track record. Moreover it is a type of yeast and will not be affected by antibiotics.
Avoid AAD
Not every illness is caused by bacteria, so if your child is sick and his paediatrician does not prescribe any antibiotics, do not insist on antibiotics. Antibiotics are not effective against viral infections.
Another reason not to demand antibiotics is the rise of ‘superbugs’, or antibiotic-resistant microorganisms. Using antibiotics when they are not needed would only worsen antibiotic resistance. Another factor that increases the rise of superbugs is antibiotic misuse, e.g. not completing your antibiotic course, or not following the antibiotic dosage.
On the other hand, if your child develops any complications (e.g. AAD) while taking antibiotics, do consult his paediatrician immediately, to see whether you should stop the antibiotic course or switch to a different antibiotic.






Comments