Atopic dermatitis, or atopic eczema, is the commonest skin disease of childhood, constitutes 40% of referrals to the Paediatric Dermatology clinic and affects 10 – 14% of children below the age of 14.
What is atopic eczema (AE)?
‘Eczema’ or dermatitis simply means skin inflammation while ‘atopic’ is a term used to describe the tendency to develop allergic conditions such as eczema, asthma, seasonal rhinitis and hay fever – which often have a genetic basis.
Atopic eczema is a chronic, relapsing, itchy skin condition that is very common in children, that often starts during the first 5 years of life (90 – 95%) but may occur at any age. Its severity can range from mild to severe and is characterised by six cardinal features:
- Dryness of skin due to underlying skin barrier defects.
- Itch-scratch cycle.
- Redness of skin due to inflammation. It may affect any area of the skin, but typically appears symmetrically on the face, neck, in front of the elbows and behind the knees.
- Onset at an early age (usually < 5 years old) and runs a chronic relapsing clinical course for years.
- Family or personal history of allergic diseases (atopic eczema, allergic rhinitis and asthma).
- Multiple environment irritants/ allergens that act as a trigger.
What causes AE?
AE is due to dynamic interaction between genetic and environmental factors. Atopic eczema tends to run in families. In a family with one allergic parent, the risk of the child developing an allergic disease is about 20 to 40 per cent. The risk increases to 60-80% if both parents are affected. Family history (genetic) is believed to play an important role, especially in families with a history of AE, asthma and hay fever.
In addition, people with AE have a genetic skin defect that allows environmental irritants and allergy-inducing substances (allergens) into their skin, which triggers inflammation.
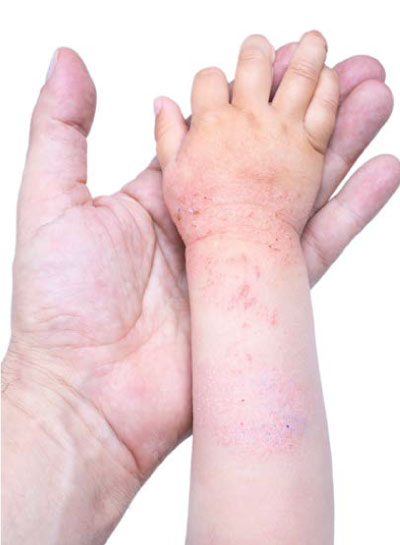
What does AE look like?
Eczema is a term that describe changes in the outer layer of the skin, which includes redness, small blisters, oozing, crusting, scaling, thickening and altered skin colour. It has many faces that changes according to its chronicity and severity of the disease.
AE can affect any part of the skin, including the face, the bends of the elbows and knees, as well as around the wrists and neck.
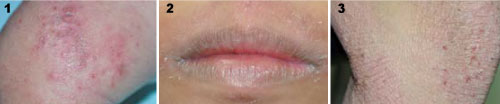
Figure 1: acute eczema with redness, blisters, erosions and crusting.
Figure 2: Subacute eczema with redness, dryness and scales.
Figure 3: chronic eczema with thickened skin, altered skin colour and scaly surface.
What can trigger AE?
Environmental triggering factors which may play a role in causing atopic eczema include the “BIG 7”
- Changes in climate
– low humidity in air conditioned indoor or hot & humid outdoor. - Salty sweat
– prolonged contact with sweat after exercise. - Harsh detergents
– prolonged and frequent hot water baths with harsh cleansers. - High bacteria load on skin
– especially Staphylococcus aureus. - Aeroallergens
– pollen, house dust mites, dog and cat dander etc. - Certain foods
– (in younger children): eggs, soy, cow’s milk, wheat and shellfish. - Stress
– certain hormones (e.g. cortisol) produced when a person is stressed or anxious triggers a chemical response in your body, which makes skin more sensitive and reactive.
Understanding that AE is a multifactorial condition will prevent parents from spending hundreds of dollars on a long list of irrelevant allergic tests. Practically, only a few patients with AE may benefit from allergy testing. Consult your doctor for further info.
Is AE contagious?
No, your child cannot get AE simply by touching or coming into close contact with someone who is affected.
Is there a way I can cure my child’s AE?
Although there is no cure for AE, most children (60-70%) grow out of AE by 7-10 years old but for some (10-20%) it may prove to be a lifelong struggle. These people can still live a normal life with a few minor changes to manage their condition.
How can AE be treated?
Treatment for atopic eczema is aimed at reducing inflammation, relieving itch and preventing future flare-ups. An important component in managing atopic eczema is to break the itch–scratch– inflammation – infection cycle.
- Combination approach:
- Improve skin hydration with a frequent moisturiser and gentle cleanser.
- An optimal shower package includes an ideal moisturiser and a gentle cleanser. The drier your skin, the more frequently you should moisturise. It is important that you choose a moisturiser you like, is cost effective with the features listed below:
– Rehydrate the skin
– Hypoallergenic and low irritation
– Contains anti-itch, anti-inflammatory and antiseptic effects
– Cost effective
– Pleasant - Anti-inflammatory measures – Steroids and Steroid sparing agents – medical devices & calcineurine inhibitors
- Anti-itch measures with wet wrap, anti-itch cream and oral anti histamine
- Antibiotic and antiseptic
- Modification of triggering factors
- Education to debunk their myths and misconceptions
- Family based approach that involves both patients and caretakers.
- Counselling about the disease, its triggers, treatment and long term prognosis.
- Empowering the patients and caretakers to apply home therapy during acute flare-ups.
An educational contribution by Malaysian Paediatric Association.





Comments