Bacterial meningitis often has severe outcomes, ranging from serious post-recovery complications such as brain damage, hearing loss, or learning disabilities. However, a more serious outcome is death, which in meningococcal meningitis happens in 1 out of 10 cases.
Vaccines are available which can control invasive meningococcal disease, namely meningococcal conjugate vaccines (MCV) and meningococcal polysaccharide vaccines.
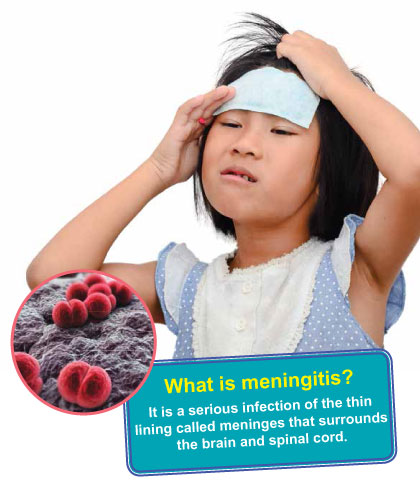
What is meningitis?
It is a serious infection of the thin lining called meninges that surrounds the brain and spinal cord.
Easy transmission
The bacteria, Neiserria meningitidis that cause this disease are easily passed from person-toperson. It spreads via:
- close contact (kissing, sneezing or coughing on someone),
- or living with an infected person (in places such as dormitories, or sharing eating or drinking utensils).
The average incubation period is four days, but can range between 2 – 10 days.
Common symptoms
There are slightly different signs/symptoms to watch out for in newborns and young children. Newborns/infants may not have the classic signs and symptoms of headache and stiff neck, or if these symptoms are present, they may present at a late stage. Here’s what you should watch out for:
- High fever
- Constant crying
- Difficult to comfort
- Excessive sleepiness or irritability
- Inactivity or sluggishness
- Poor feeding
- A bulging fontanelle (the soft spot on a baby’s head)
- Stiffness in a baby’s body and neck
The following signs and symptoms may occur in children older than two years old:
- Sudden high fever
- Severe headache
- Stiff neck
- Vomiting or nausea with headache
- Confusion or difficulty concentrating
- Seizures
- Sleepiness or difficulty waking up
- Sensitivity to light
- Lack of interest in drinking and eating
- Purpuric rash
Factors that increase the risk of meningitis:
- Age – the young (e.g. infants, toddlers), adolescents, and the elderly are at higher risk from infection with Neisseria meningitidis.
- Location – places where large groups of people gather often make it easier for this disease to spread.
- Travel – visiting places that are endemic to meningitis exposes you to the bacteria. This includes the ‘meningitis belt’ in the sub-Saharan African region and travellers to Mecca during the annual Hajj and Umrah pilgrimage.
Prevention is better than cure!
Catching it early means a 90% chance of survival. However, there may be long-lasting (or even permanent) complications. The best thing to do is to prevent meningococcal meningitis by immunising against it. There are two ‘types’ of vaccines:
- The “old” meningococcal vaccine is polysaccharide-based. It is only effective in children above two years, has poor immune memory, and does not contribute to herd immunity.
- The newer meningococcal conjugate vaccines (MCV) protect children from six weeks onwards, induce immune memory, and confer protection to the community.
Vaccination should be seriously considered in order to protect your children, adolescents and the elderly from this very debilitating and not infrequently fatal disease.
An educational contribution by Malaysian Paediatric Association.




Comments