Modern medical practice encourages regular antenatal examinations (every four weeks or so) starting around your 11th week. During the first check-up, the doctor takes your medical history along with your partner’s, as well as those of both your families. A physical examination is conducted with your weight, height, heart rate and blood pressure measurements recorded. The doctor will also check on other organs, including lungs, heart and breasts. A blood test will reveal your blood group and whether you are immune to illnesses such as Hepatitis B and rubella (German measles).
A urine test is done to detect the presence of protein, sugar or evidence of infection. During subsequent check-ups, the doctor will measure your weight and blood pressure again. The most important thing to know is whether you and baby are in good health. As the pregnancy progresses, the doctor will keep track of baby’s growth, size, position in the womb and activity. Your doctor will tell you whether you are likely to need to deliver by Caesarean section and what other preparations you can make for birth.
The Ultrasound Scan
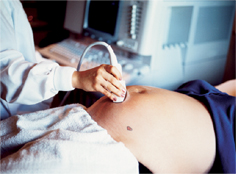
Until the 1970s, doctors had no means of looking into the womb to check on the developing foetus. With the advent of ultrasound scanning, doctors could monitor foetal growth and detect abnormalities, then help parents make informed decisions about treatment. Ultrasound is completely safe to mother and baby. A device called a transducer is run over mother’s abdomen, bouncing sound waves off the inside of the womb. The result is a blackand- white image of the foetus projected on a screen.
The following table shows when ultrasound scans are typically conducted and why.
| When in pregnancy | Why conducted | What it detects |
| Below 12 weeks | Personal reassurance for parents |
|
| Mother experiences pain or bleeding |
|
|
| Weeks 18-20 | To check that foetus is growing and normal |
|
When To Raise The Alarm
Apart from morning sickness, heartburn and some minor changes to your physical appearance, pregnancy should not make you feel unwell or manifest extreme symptoms. If you experience any of the following, see your doctor as soon as possible.
- Heavy vaginal bleeding or spotting, lasting more than a day and/or is accompanied by fever, chills or pain
- Persistent headaches accompanied by dizziness or faintness
- Pain in the pelvic area
- Vomiting if it occurs more than two or three times a day, and if it is accompanied by pain or fever
- Fever
- Painful urination
- Steady or heavy discharge of watery fluid from vagina
- Sudden swelling in ankles, hands and face
- “Visual disturbances” – sudden dimness, blurring or temporary blindness
Responding to Your Test Results
What happens if your doctor says there might be a problem in your pregnancy? Stay calm, and:
- Ask questions. Ask the doctor to explain the condition that your foetus has or is at risk of having, baby’s life expectancy and what problems he may have, physically and mentally. It may be difficult now, but it’s better to be prepared.
- Do your own research. Ask your doctor to refer you to experts on that condition, read books and articles about it, and try to make contact with parents of children who have it.
- Count your blessings. This is especially hard to do, but remember that with advances in medical screening and treatment technology, baby has a far better prognosis than a child born with the same condition as recently as 10 years earlier.






Comments