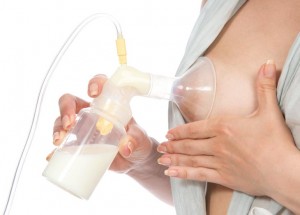
Experts have agreed that breast milk is both highly nutritious and acts as a natural antibiotic that helps the baby fight off numerous types of infections. Breastfeeding should also be rewarding and relaxing for both the mother and the baby, however, some complications can arise during breastfeeding that may discourage mothers to continue feeding their child. These are some of the most frequently asked questions (FAQs) by new mothers:
Are my nipples supposed to feel sore and dry during or after breastfeeding?
No, most experts agree that any sensation of soreness or cracking of the nipples are caused by the baby’s poor-positioning during feeding and the use of hygiene (soaps, creams, etc.), products on the breast before, during or after breastfeeding.
Latching and positioning is the key, ensure proper latching and use your finger to break suction. Optionally, you can apply lanolin after feeding as it provides protection and care for your skin whilst preventing over-drying of your nipples. You could also apply your own breast milk around the nipples after feeding your baby. During feeding, you can also alternate between nipples and let them air-dry between each feeding session. Experiencing soreness of the nipples for the first few days is normal, it gets easier as your body adjusts.
I understand that my body is producing milk during this time and this causes my breast to enlarge. But why does it feel hard, painful and swollen?
Having your breasts full of nutritious milk for your baby is both natural and healthy. However, if not emptied regularly the blood vessels situated in the breast become congested, which in turn traps fluids within the breast tissue causing engorgement. Nipples may flatten if engorgement is allowed to persist causing poor-latching and further discomfort.
Engorgement usually happens on the 3rd – 5th day after birth. Feed your baby regularly and avoid missing feeding times. You can also express your milk manually or via pump, massage while running warm water over your breast can also work to soothe when in pain. Coincidently, you can also prevent blocked ducts using the same technique.
One of my breasts feels sore, achy, hot and tender-like, often following up is a fever, can I continue to breastfeed or should I wait for the fever to go away before breastfeeding again?
The symptoms described are similar to when a mother’s breast is bacterially-infected. Scientifically referred to as Mastitis or breast infection, the breast may feel swollen, a hot sensation builds up on one breast and pain accumulates. Symptoms seem similar to the ones suffered during engorgement or plugged ducts and is often perpetrated by high-stress and/or fatigue.
Preventing mastitis can be done by continuous breastfeeding or expression of milk on a timely basis. If you are infected, don’t stop breastfeeding the baby, your milk shouldn’t be infected and thus won’t affect your child. Don’t wait for the fever to go away, you should visit your local pediatrician/lactation consultant for further treatment.
Can I breastfeed my baby if I have a fungal infection?
Yes, however, you should visit your doctor for immediate treatment for both you and your baby. Fungal infection of the nipple or “Thrush”, is a common occurrence triggered by a build-up of Candida bacteria around your nipples. If you’re already infected, make sure you clean all your stuff that has either come into contact with you or your baby thoroughly, soaking in hot water usually suffices. Another tip is to change nursing pads regularly and keep your nipples air-dry.
Mothers often have had to deal with these and other intimate and personal concerns alone and this adds to the pressure. Husbands, partners and other immediate family members should play a role in providing much needed emotional, psychological and physical support.
Learning the proper techniques in breastfeeding may also help you better hone your maternal skill sets. Support groups, pediatricians, lactitions, maternal consultants and even family and friends can help you through your breastfeeding debacles.
An educational contribution by Malaysian Paediatric Association.






Comments