Congenital defects of the heart can either be induced externally through environmental factors such as maternal smoking or alcohol consumption as well as be genetically-driven (i.e. Trisomy 21 [Down Syndrome] or Trisomy 18 [Edward Syndrome]). Infants may show signs of heart failure early if there is a large hole in the heart. Some may be blue due to reversal of blood flow that bypasses the lungs. Heart failure presents with breathlessness during feeding.
Some mothers may feel a little apprehensive about breastfeeding their child for fear that it may worsen the severity of their child’s symptoms or provoke an attack. The following are some of the more widespread misconceptions of breastfeeding a CHD infant:
Misconceptions
1. CHD infants can only feed exclusively on formula.
- Studies suggest breast milk effectiveness is enhanced in premature or ill-affected infants. Breast milk is also easily digested and contains antibodies that most formulas can’t offer.
- Usually involves combination of formula, supplements and breast milk.
- Hospitals will consult on options for feeding the baby. Ultimately, the current condition of the infant will dictate the best possible option.
2. Breastfeeding tires CHD infants more quickly as opposed to bottle feeding.
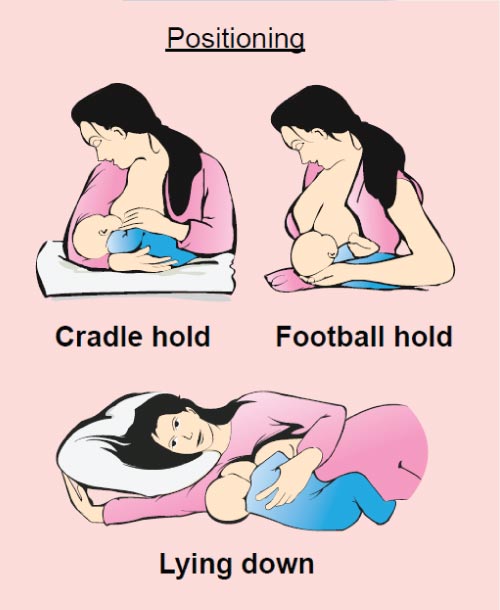
- Experts have agreed that suckling, swallowing and breathing is relatively easier when a baby is breastfeeding provided the techniques used are sound (proper latching and positioning).
What is proper latching/attachment?
Baby’s mouth covers the whole nipple, her chin and nose are touching your breast. You can hear her swallow and the experience feels comfortable. Breastfeeding shouldn’t hurt your nipple.
3. CHD infants under intensive care units cannot be fed breast milk.
- Expressed breast milk can be fed to the infant while in intensive care with added supplements.
- Helps mothers feel involved in the development of the child in the ICU.
- Short but periodically frequent breast feeding during the day and pump your milk when you can so that if you are unable to breastfeed your baby due to restrictions (i.e. baby placed in incubator) then the milk can be fed to her through tubes.
- In any case, your milk can still be stored and used when the baby is ready. Expressing your milk will also prevent from complications such as engorgement, thrush or mastitis of the breasts.
4. Bottle-fed babies get better faster.
- Studies have shown breastfed CHD infants gain weight more quickly than their bottle fed counterparts. Antibodies in the breast milk also help babies fight against infections. This translates into shorter stays at hospitals.
- Severity of the disease has nothing to do with, and neither is it affected by, breastfeeding.
Since breastfeeding is an activity that further strengthens the bond between mother and child, missing out may affect mothers emotionally. Therefore, resilience and persistence of the supporting family unit including immediate family members and friends is vital. There is no substitute for the rich goodness of a mother’s breast milk for a newborn. However, don’t feel discouraged or inferior if you can’t breastfeed your baby as often, what’s even more important to consider during this juncture is that the baby receives proper medical treatment for his/her heart condition.
An educational contribution by Malaysian Paediatric Association.





Comments