For many women, the third trimester is a period of tiredness, aches and pains before the excitement of baby’s arrival. You may have begun feeling strong ‘false’ contractions as your body prepares for the big day. You, too, can prepare by finding out about the different birth methods, your choices for pain relief in labour and birth, and possible complications that could occur. Remember, of course, that with today’s advanced medical facilities, you have high chances of delivering a healthy baby with a minimum of trouble.
Which way out?
Many women see ‘natural’ (vaginal) childbirth as their only option. Doctors agree that this is still the safest method, unless either mother or baby has health complications that will make natural birth dangerous.
Sometimes, the doctor may recommend a planned Caesarean section (surgery to deliver the baby through a cut made in the abdomen and uterus) for various reasons, including:
- Baby in breech position
- Prolonged labour
- Drop in baby’s heart rate
- Not enough room in the birth canal
- Maternal health conditions (eg high blood pressure)
How will I know when it’s time?
Many first-time mothers are anxious about whether they will know when they really are in labour. After giving birth, most say that when labour began, there was no mistaking it! These are some of the signs that it’s time for baby to make his big appearance:
- Painful contractions
- Show (bloody mucus discharge)
- Breaking of water bag (usually with a gush)
- Indigestion
- Diarrhoea
- Nausea & vomiting
- ‘Lightening’ feeling
You need not wait for all of these symptoms before you go to the hospital or maternity centre. As soon as you think you’re in labour, make your way there. A false alarm may be embarassing, but at least the doctor will be able to check that all is well before sending you home to wait a little longer.
Labour
The actual labour process occurs in three stages:
- The first stage of labour describes the stage between the onset of labour and when your cervix is fully dilated.
- The second stage is the most tiring part of labour, because it is the actual delivery. You will need to ‘help’ baby out by pushing during contractions. Between contractions, relax and don’t try to push because it will only tire you out. It will not help baby emerge faster!
- The third stage occurs after baby is out. The placenta, which has now completed its work of furnishing baby with nutrient and oxygen supplies and removing waste from his body, is now expelled in another series of contractions.
Occasionally, in the second stage of labour, delivery of the baby may need to be assisted by the doctor, using forceps or vacuum extraction, for reasons such as a prolonged or repeated drop in the baby’s heart rate, or the second stage taking far too long, hence exhausting the mother and baby. In some cases, before labour begins naturally the doctors may induce it (begin it artificially) because of any of the following reasons:
- Past due date
- Membrane has broken, but labour has not started
- Labour is progressing too slowly
- Baby is smaller than he should be at this stage
- Complications, eg high blood pressure or diabetes mellitus in the mother
Pain Relief
You may feel pressured by expectations that you need to refuse all forms of pain relief in labour in order to avoid being labelled ‘weak’. Sadly, this belief that pain in childbirth must be endured without medical intervention is still very common in Malaysia. By knowing the truth about the different forms of pain relief, you can decide now whether you want it when in labour. Even if you don’t, try to decide which is best for you so that if you need to change your mind in the delivery room, the decision will already have been made. Giving birth is an intense, unique experience, so do what you can to give yourself good memories of it.
There are several options of pain relief available. This is only a brief introduction; you still need to discuss this with your doctor and decide which one to opt for. Each of these methods has benefits and drawbacks, and you should be the one to weigh everything and make the decision because it affects you most.
- Opiate injection – An injection of painkiller is given, usually into the muscle in the buttock area
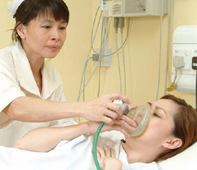
- Entonox inhalation – A combination of oxygen and nitrous oxide is breathed in using a face mask during contractions
- Epidural injection – A hollow needle is inserted between two vertebrae (parts of the backbone) into the epidural space, and a plastic tube is threaded through the needle. Anaesthetic solution is fed through the tube throughout the rest of the labour and delivery.
Episiotomy
When baby’s head crowns or begins to appear, there is a risk of the perineum (area between the vulva and rectum) tearing. If the doctor feels that the risk of tearing is great, episiotomy may be necessary. This is a cut in the perineum, made under local anaesthetic, to prevent tearing (which is less easily controlled). Whether a tear has occurred or episiotomy has been performed, the doctor will repair the area with stitches after birth. Often, with second or subsequent childbirth, episiotomy may not be necessary.
Caesarean section
The doctor may advise Caesarean section sometime during your pregnancy, or in the delivery room, due to any of these reasons:
- baby in breech position (ie buttocks or legs at the bottom)
- labour is prolonged without progress
- baby’s heart rate drops during birth
- birth canal too narrow
- your health conditions, eg high blood pressure
Did you know?
Caesarean sections date back to the days of the Roman empire. A law called the lex caesar stated that if a woman in labour was sure to die, an operation was to be performed to save her baby. It was seen as a heroic measure to preserve one life rather than allowing two deaths to occur. Today, thanks to safe surgical methods, skilled surgeons and modern medical equipment, the Caesarean section is seen as a means of saving mother’s life as well as baby’s and, more often than not, it is performed for the safety of both.






Comments